Sulbactam for Treatment of Carbapenem-Resistant Acinetobacter baumannii
This is a challenging pathogen, requiring pharmacokinetic and pharmacodynamic considerations; the recent FDA approval of sulbactam-durlobactam offers new hope.
This is a medical illustration of carbapenem-resistant, Acinetobacter sp. bacteria. Illustration credit: Dan Higgins; James Archer
Unlike other traditional β-lactamase inhibitors, sulbactam has intrinsic antibacterial activity against Acinetobacter baumannii through its ability to inhibit cell wall synthesis by binding to penicillin-binding proteins (PBP1a, PBP1b, and PBP3).1 Sulbactam is with ampicillin as a fixed 2:1 ratio of ampicillin to sulbactam and an approved dose of up to 3 g (2 g ampicillin and 1 g sulbactam) every 6 hours. The Clinical and Laboratory Standards Institute (CLSI) breakpoints for ampicillin-sulbactam are also reported as a 2:1 ratio of ampicillin to sulbactam and for A baumannii are listed as susceptible at minimum inhibitory concentration (MIC) values less than or equal to 8/4 mg/L, intermediate at an MIC of 16/8 mg/L, and resistant at MIC values equal to or greater than 32/16 mg/L. However, activity of ampicillin-sulbactam against A baumannii is mediated by sulbactam alone.2 This is problematic as both the labeled dosing of ampicillin/sulbactam and the subsequent susceptibility breakpoints for A baumannii were selected based on ampicillin, the inactive component. Therefore, clinicians need to appreciate that an MIC value of 8/4 mg/L to ampicillin/sulbactam reflects a sulbactam MIC of 4 mg/L, and that CLSI susceptibility breakpoints are not necessarily appropriate based on labeled dosing. Thus, a critical dive into sulbactam in vitro activity and pharmacokinetics (PK) and pharmacodynamics (PD) is essential for appropriate use of sulbactam in A baumannii infections.
IN VITRO ACTIVITY OF SULBACTAM
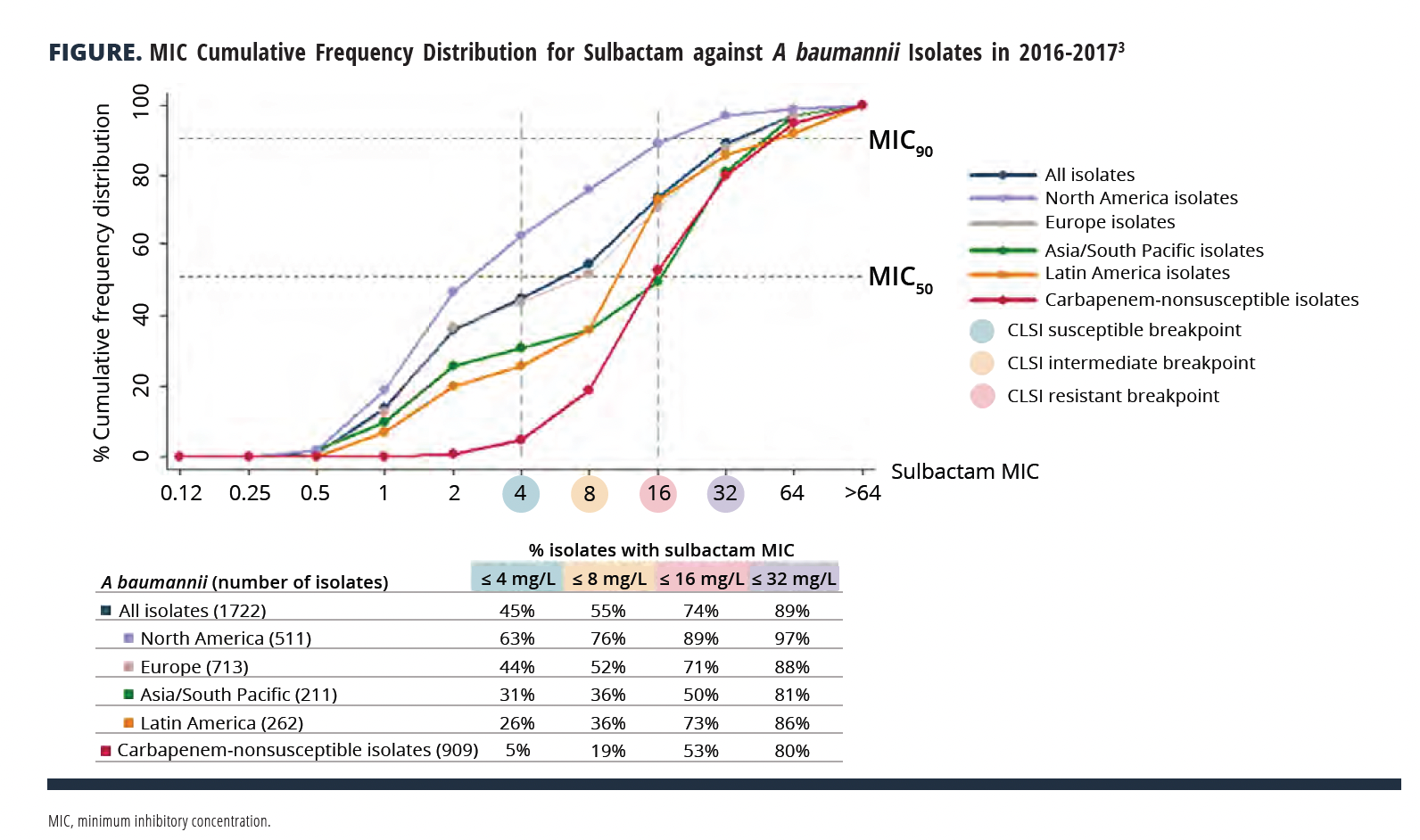
The MIC distribution of sulbactam was tested in an in vitro surveillance study in 2016-2017 evaluating 1722 isolates of A baumannii collected globally.3 The sulbactam MIC distributions were consistent between most geographic regions with sulbactam MIC50/MIC90 values of 8 mg/L and 64 mg/L, respectively. Interestingly, MIC distributions were lower in North America, where MIC50 and MIC90 values of 2 mg/L and 32 mg/L, respectively, were demonstrated. If CLSI breakpoints are applied, 45% of isolates globally and 63% in the United States would be considered susceptible.
In this surveillance study, roughly 50% of all A baumannii isolates were carbapenem resistant (CRAB). MIC distributions of sulbactam were higher in CRAB with MIC50/MIC90 values of 16 mg/L and 64 mg/L, respectively. If CLSI breakpoints are applied, only 5% of CRAB isolates are susceptible to sulbactam (FIGURE3). However, as mentioned, susceptibility breakpoints are based on ampicillin, highlighting the need for PK/PD assessment of sulbactam to identify what, if any, role this agent has for CRAB.
SULBACTAM PHARMACOKINETICS
Sulbactam displays dose-dependent pharmacokinetics, with an average peak serum concentration of 43 mg/L after a 30-minute infusion of 1 g in healthy volunteers. The serum half-life is 1 hour, with elimination primarily by glomerular filtration and tubular secretion.4 The half-life is not altered significantly until creatinine clearance is less than 30 mL/min and a decrease in dosage is required.5 Sulbactam demonstrates moderate plasma protein binding of 38%, which is not expected to have a dramatic impact on PK parameters in patients with hypoalbuminemia. Favorable penetration of sulbactam has been demonstrated into various sites including the lower respiratory tract, the most common site of infection caused by A baumannii.6-8 The epithelial lining fluid (ELF) penetration ratios of sulbactam in healthy subjects were 0.50 and 0.81, based on total and unbound plasma concentrations to ELF concentrations, respectively.8
SULBACTAM PHARMACODYNAMICS
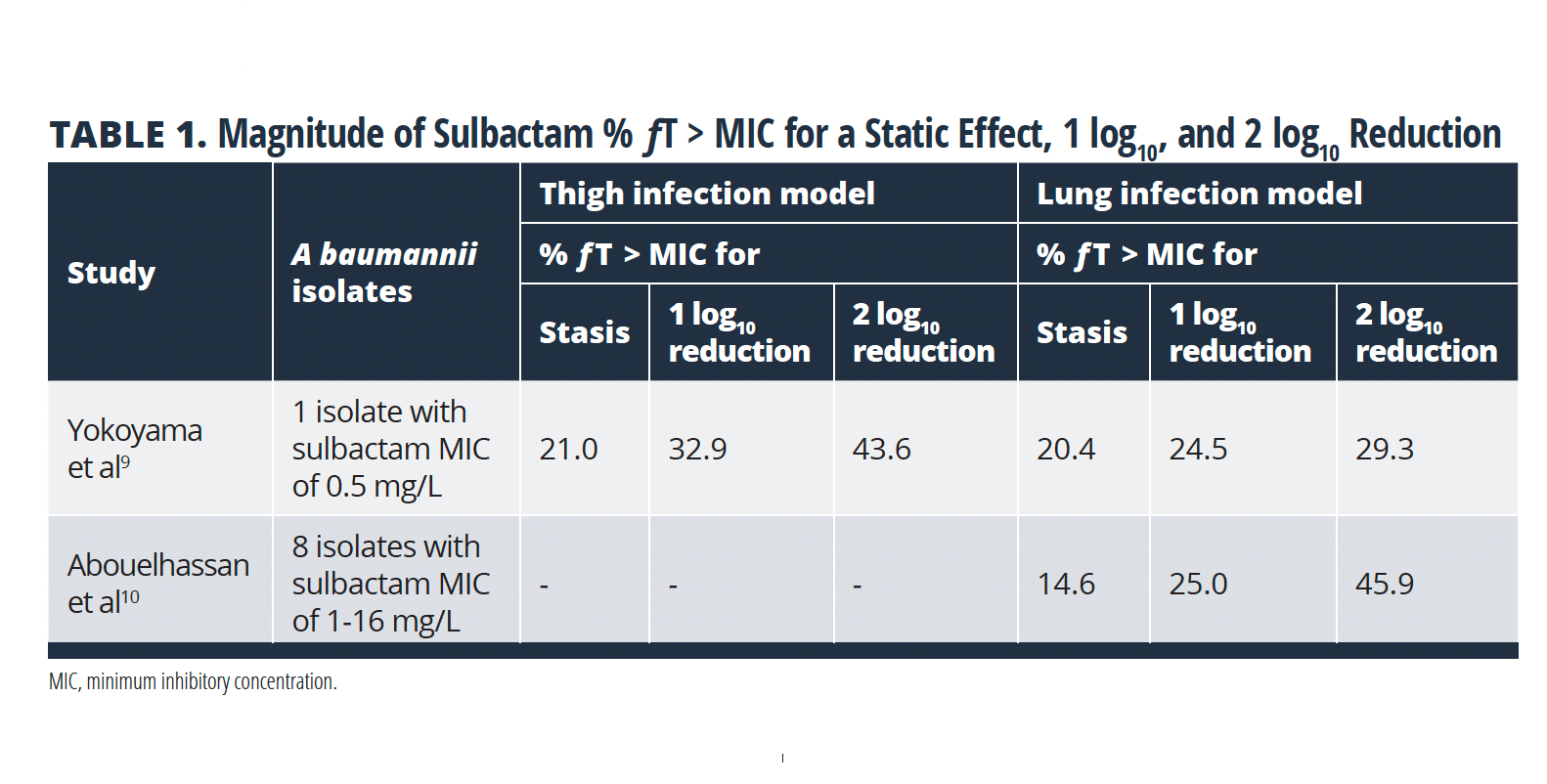
The percentage of time that unbound plasma concentrations remain above the MIC (% ƒT > MIC) is the PK/PD parameter that best correlates with sulbactam’s activity against A baumannii.9,10 The magnitudes of ƒT > MIC associated with sulbactam efficacy against various strains of A baumannii have been investigated in 2 neutropenic lung9,10 and 1 neutropenic thigh9 models (TABLE 1). The ƒT > MIC targets that correlate with activity of sulbactam were similar in both lung infection models, with a ƒT > MIC of 25% being associated with a 1 log10 reduction in CFU over 24 hours. A slightly higher ƒT > MIC target of 33% was required for a 1 log10 reduction in the thigh infection model; however, only 1 isolate was assessed in this model, and these data are generally consistent with the lung model.

PHARMACOKINETIC AND PHARMACODYNAMIC DOSE OPTIMIZATION FOR SULBACTAM
To determine the optimal dosing regimen of sulbactam, 2 Monte Carlo simulations and probability of target attainment (PTA) analyses were performed based on PK data from 16 patients treated with sulbactam with ventilator-associated pneumonia.10,11 Those results are summarized in TABLE 2.10,11 With the upper end of the package insert dose of ampicillin-sulbactam (3 g every 6 hours with intermittent infusion, equivalent to sulbactam 4 g/d), PTA of 90% or more is achieved for A baumannii with sulbactam MIC less than or equal to 4 mg/L when the 1 log10 reduction target of 25% ƒT > MIC is considered. However, this dosage is inadequate for A baumannii with sulbactam MIC greater than 4 mg/L, which account for 95% of CRAB.
Dosing simulations were performed to assess whether alternate dosing strategies could achieve 90% or greater PTA at higher MIC values. At a sulbactam MIC of 8 mg/L, simulations demonstrated that either a 4-hour infusion of ampicillin-sulbactam 3 g every 6 hours (sulbactam 4 g/d) or an intermittent infusion of ampicillin-sulbactam 3 g every 4 hours (sulbactam 6 g/d) achieved 90% or greater PTA. At a sulbactam MIC value of 16 mg/L, higher ampicillin-sulbactam doses of 9 g every 8 hours (sulbactam 9 g/d) administered by 4-hour infusions are necessary to provide 90% or greater PTA. Higher doses than currently recommended12 are necessary to achieve PK/ PD targets at an MIC of 32 mg/L, although these analyses did not assess the ability of 9 g/d as a continuous infusion to achieve targets at this MIC value.
Taken together, these data suggest that the CLSI susceptibility breakpoint of 4 mg/L of sulbactam (ie, 8/4 mg/L ampicillin/sulbactam) is appropriate with labeled dosing as an intermittent infusion. Isolates that are currently considered intermediate can be targeted by either prolonging the infusion or administering ampicillin/sulbactam as a 3-g dose every 4 hours. Additionally, larger doses of 9 g every 8 hours of ampicillin/sulbactam administered as a prolonged infusion, as recommended in the Infectious Diseases Society of America guidance document for the management of drug-resistant gram-negative infections, provides 90% or greater PTA for A baumannii isolates with low-level resistance (sulbactam MIC of 16 mg/L).
SULBACTAM HAS ISSUES; DURLOBACTAM TO THE RESCUE?
Even with dose optimization, the PK/PD targets of sulbactam cannot be reliably attained in nearly half of CRAB isolates due to high sulbactam MICs (≥ 32 mg/L). Additionally, although PK/ PD targets can be reached for isolates with MIC values of 16 mg/L with aggressive dosing strategies, data suggesting ampicillin-sulbactam can be successfully clinically used at high doses for isolates with these MIC values are lacking. Moreover, due to automated susceptibility testing limitations, clinicians are likely only to know that MIC values for a resistant isolate are equal to or greater than 16 mg/L. Given that most isolates in this category will have MIC values greater than 16 mg/L, decisions that can be made based on antimicrobial susceptibility testing reporting are limited. Furthermore, preliminary data suggest that a higher ƒT > MIC target of 60% may be needed for sulbactam-resistant (MIC ≥ 16 mg/L) CRAB isolates when compared to either sulbactam or carbapenem-susceptible A baumannii, and that those targets cannot be reliably achieved with 9 g/d of sulbactam.13,14
It is in this backdrop that the recently FDA approved combination, sulbactam-durlobactam, has provided a new hope for treating infection caused by A baumannii. Durlobactam is a diazabicyclooctane β-lactamase inhibitor with potent inhibitory activity against class D OXA β-lactamases (OXA-23, OXA-24/40), which are the primary mechanisms involved in sulbactam and carbapenem resistance in A baumannii.15 The addition of durlobactam has been shown to restore the activity of sulbactam and lower the MIC90 from 64 mg/L to 2 mg/L. Indeed, 96% of tested CRAB isolates had a sulbactam-durlobactam MIC less than or equal to 4/4 mg/L, the recently approved CLSI susceptibility breakpoint.3
The efficacy and safety of sulbactam-durlobactam vs colistin, both in combination with imipenem, for treatment of pneumonia or bloodstream infection caused by A baumannii was evaluated in a phase 3, multicenter, randomized controlled study (NCT03894046).16 In this trial, sulbactam-durlobactam demonstrated noninferiority to colistin for the primary end point of 28-day all-cause mortality (19% vs 32%; difference –13% [95% CI, –30.0 to 3.5]) and superiority in clinical cure rates (62% vs 40%; difference 22% [95% CI, 2.9 to 40.3]) in patients with CRAB infections. Sulbactam-durlobactam was also associated with a lower incidence of nephrotoxicity, compared with the colistin group (13% vs 38%; P < .001). This trial represents the first well-controlled study demonstrating improved clinical outcomes of any agent when compared to colistin for CRAB. The increased in vitro activity and potency combined with clinical trial data support preferred usage of sulbactam-durlobactam over high-dose ampicillin-sulbactam–based combinations once it becomes commercially available.
References
- Papp-Wallace KM, Senkfor B, Gatta J, et al. Early insights into the interactions of different β-lactam antibiotics and β-lactamase inhibitors against soluble forms of Acinetobacter baumannii PBP1a and Acinetobacter sp. PBP3. Antimicrob Agents Chemother. 2012;56(11):5687-5692. doi:10.1128/AAC.01027-12
- Higgins PG, Wisplinghoff H, Stefanik D, Seifert H. In vitro activities of the beta-lactamase inhibitors clavulanic acid, sulbactam, and tazobactam alone or in combination with beta-lactams against epidemiologically characterized multidrug-resistant Acinetobacter baumannii strains. Antimicrob Agents Chemother. 2004;48(5):1586-1592. doi:10.1128/AAC.48.5.1586-1592.2004
- McLeod SM, Moussa SH, Hackel MA, Miller AA. In vitro activity of sulbactam-durlobactam against Acinetobacter baumannii-calcoaceticus complex isolates collected globally in 2016 and 2017. Antimicrob Agents Chemother. 2020;64(4):e02534-19. doi:10.1128/AAC.02534-19
- Foulds G, Stankewich JP, Marshall DC, et al. Pharmacokinetics of sulbactam in humans. Antimicrob Agents Chemother. 1983;23(5):692-699. doi:10.1128/AAC.23.5.692
- Wright N, Wise R. The elimination of sulbactam alone and combined with ampicillin in patients with renal dysfunction. J Antimicrob Chemother. 1983;11(6):583-587. doi:10.1093/jac/11.6.583
- Brown RM, Wise R, Andrews JM, Hancox J. Comparative pharmacokinetics and tissue penetration of sulbactam and ampicillin after concurrent intravenous administration. Antimicrob Agents Chemother. 1982;21(4):565-567. doi:10.1128/AAC.21.4.565
- Wise R, Donovan IA, Andrews JM, Drumm J, Bennett S. Penetration of sulbactam and ampicillin into peritoneal fluid. Antimicrob Agents Chemother. 1983;24(2):290-292. doi:10.1128/AAC.24.2.290
- Rodvold KA, Gotfried MH, Isaacs RD, O’Donnell JP, Stone E. Plasma and intrapulmonary concentrations of ETX2514 and sulbactam following intravenous administration of ETX2514SUL to healthy adult subjects. Antimicrob Agents Chemother. 2018;62(11):e01089-18. doi:10.1128/AAC.01089-18
- Yokoyama Y, Matsumoto K, Ikawa K, et al. Pharmacokinetic/pharmacodynamic evaluation of sulbactam against Acinetobacter baumannii in in vitro and murine thigh and lung infection models. Int J Antimicrob Agents. 2014;43(6):547-552. doi:10.1016/j.ijantimicag.2014.02.012
- Abouelhassan Y, Kuti JL, Nicolau DP, Abdelraouf K. 1652. Sulbactam against Acinetobacter baumannii pneumonia: pharmacokinetic/pharmacodynamic appraisal of current dosing recommendations. Open Forum Infect Dis. 2022;9(suppl 2). doi:10.1093/ofid/ofac492.118
- Jaruratanasirikul S, Nitchot W, Wongpoowarak W, Samaeng M, Nawakitrangsan M. Population pharmacokinetics and Monte Carlo simulations of sulbactam to optimize dosage regimens in patients with ventilator-associated pneumonia caused by Acinetobacter baumannii. Eur J Pharm Sci. 2019;136:104940. doi:10.1016/j.ejps.2019.05.018
- Tamma PD, Aitken SL, Bonomo RA, Mathers AJ, van Duin D, Clancy CJ. Infectious Diseases Society of America 2023 guidance on the treatment of antimicrobial-resistant gram-negative infections. Infectious Diseases Society of America. June 7, 2023. Accessed June 22, 2023. https://www.idsociety.org/practice-guideline/amr-guidance/
- Abouelhassan Y, Kuti JL, Nicolau DP, Abdelraouf K. Sulbactam for Acinetobacter baumannii pneumonia: stratification of pharmacokinetics/pharmacodynamics targets according to carbapenem susceptibility. Presented at: ASM Microbe 2023; June 15-19, 2023; Houston, TX. Accessed June 24, 2023.
- Abouelhassan Y, Nicolau DP, Abdelraouf K. BlaOxa-23 is a predictor of lack of sulbactam efficacy against Acinetobacter baumannii pneumonia. Presented at: ASM Microbe 2023; June 15-19, 2023; Houston, TX. Accessed June 24, 2023.
- Durand-Réville TF, Guler S, Comita-Prevoir J, et al. ETX2514 is a broad-spectrum β-lactamase inhibitor for the treatment of drug-resistant gram-negative bacteria including Acinetobacter baumannii. Nat Microbiol. 2017;2:17104. doi:10.1038/nmicrobiol.2017.104
- Kaye KS, Shorr AF, Wunderink RG, et al. Efficacy and safety of sulbactam-durlobactam versus colistin for the treatment of patients with serious infections caused by Acinetobacter baumannii-calcoaceticus complex: a multicentre, randomised, active-controlled, phase 3, non-inferiority clinical trial (ATTACK). Published online May 11, 2023. Lancet Infect Dis. 2023;S1473-3099(23)00184-6. doi:10.1016/S1473-3099(23)00184-6

Newsletter
Stay ahead of emerging infectious disease threats with expert insights and breaking research. Subscribe now to get updates delivered straight to your inbox.
