Antiviral Drug Tecovirimat May Shorten Duration of Monkeypox Illness
A recent study in the United Kingdom suggests that more research into the possible benefits of antiviral drug tecovirimat for treating monkeypox may be warranted after showing positive results in one patient.
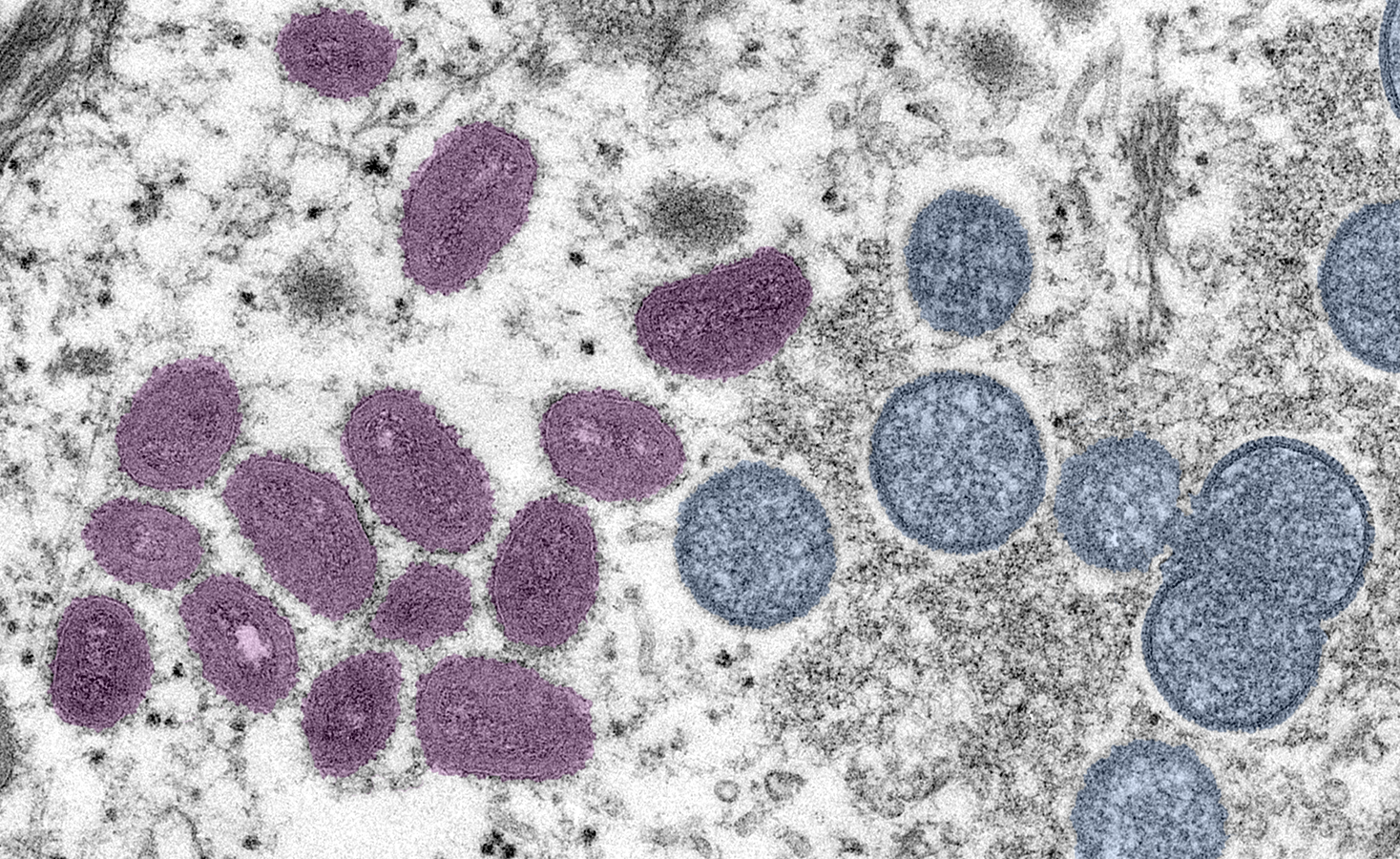
The antiviral drug tecovirimat may improve outcomes for people infected with monkeypox, a recent study in Britain suggests.
The small retrospective observational study, published in The Lancet Infectious Diseases, included 7 patients who were treated for monkeypox at high consequence infectious diseases centers in Britain between Aug. 15, 2018, and Sept. 10, 2021 and aimed to describe the clinical course of the disease and response to novel antiviral therapies.
“The single biggest takeaway is the excellent clinical and virological response to the oral antiviral tecovirimat in one patient with monkeypox who received this agent,” lead author Hugh Adler, PhD, of Liverpool University Hospitals NHS Foundation Trust told Contagion. “We definitely need well-powered, prospective studies to validate this finding, but it is a strong signal, and may be of use to clinicians managing patients with monkeypox in the current outbreak in the Western Hemisphere.”
Three patients were treated with 200 mg of brincidofovir weekly before developing elevated liver enzymes and ending treatment. One patient received 600 mg of tecovirimat twice a day for two weeks and experienced a shorter duration of illness and viral shedding.
The study included patients who tested positive after traveling from Nigeria along with transmission to a healthcare worker and within a family household. All seven of the patients in the study developed skin lesions, and all made a full recovery.
“We were surprised to find positive monkeypox PCR results in blood and upper respiratory swabs, and particularly surprised that the throat swabs remained PCR positive long after the resolution of the rash in some cases,” Adler said. “We don't yet know the implications for infection control advice, etc. (after all, don't forget that patients with COVID can remain PCR positive for weeks despite no longer being infectious), but it merits consideration when managing patients in the current outbreak, and warrants dedicated research (eg with viral culture) to settle the question once and for all.”
Three patients in the study spent more than three weeks in isolation because of prolonged positivity. The disease was mild in all of the patients involved in the study, with none experiencing pneumonia or sepsis. Unexpected symptoms included mild relapse six weeks after discharge in one patient and a deep tissue abscess that required drainage in another. Isolation led to low mood in patients.
“We wanted to draw attention to the prolonged illness and hospitalization our patients experienced, even with ultimately ‘uncomplicated’ monkeypox, so that healthcare providers can prepare to psychologically support patients with this infection, and for policymakers to consider whether self-isolation at home is an option for selected patients,” Adler said. “And most importantly, we want healthcare providers and readers everywhere to know that monkeypox remains a significant public health problem in West and Central Africa, where there is an urgent unmet need for antiviral treatments, vaccines and more evidence-based infection control protocols.
Monkeypox is endemic in Africa, but global health officials have been closely monitoring the recent outbreak of the disease outside of Africa. About 300 cases of monkeypox have been reported in a dozen countries.
“Clinicians, including the authorship of this paper, remain involved in the clinical and public health response to the ongoing unprecedented monkeypox outbreak in the UK, Europe and beyond, and I am confident that this will be brought under control,” Adler said. “There are plans to undertake further research to explain our finding of positive monkeypox viral PCR testing in upper respiratory throat swabs and understand the infection control implications of this. And internationally I am pleased that there is a trial recruiting in the Democratic Republic of the Congo looking at the role of smallpox vaccination for healthcare staff caring for patients with monkeypox, and an expanded access program for tecovirimat in the Central African Republic.”
Newsletter
Stay ahead of emerging infectious disease threats with expert insights and breaking research. Subscribe now to get updates delivered straight to your inbox.
2 Commerce Drive
Cranbury, NJ 08512
All rights reserved.
