Should Cefazolin be Prescribed in Patients With B-lactam Allergies?
For patients undergoing surgery, looking at the potential benefits of this antimicrobial for prophylaxis.

The Clinical Practice Guidelines for Antimicrobial Prophylaxis in Surgery, released in 2013, recommends use of cefazolin as a first line for orthopedic surgeries including total joint replacement procedures. In the case of beta-lactam allergies, patients may receive either clindamycin or vancomycin.1 A 2023 National Healthcare Safety Network (NHSN) reports an estimated $3.3 billion annual cost nationwide and increased hospital length by approximately 10 days as a result of any surgical site infections (SSI).2 Cefazolin is preferred due its more reliable activity against Gram-positive bacteria and is associated with less adverse effects compared with clindamycin or vancomycin.3,4
Almost 75% of patients acquire penicillin allergy labels by the age of three. However, Romano and colleagues in 2014, found that patients lose beta-lactam allergies over time based on skin hypersensitivity tests. Approximately 90% of all patients with benign reactions would not react to the same skin test challenge after 3 years.5 Additionally, a 2019 study found comparing cefazolin with non-cefazolin regimen for surgical prophylaxis in orthopedic surgeries found that prosthetic joint infections were significantly higher when non-cefazolin regimen were used perioperatively.6 Therefore, the purpose the study, “cefazolin vs second-line antibiotics for surgical site infection prevention after total join arthroplasty among patients with a beta-lactam allergy,” was to evaluate the incidence of skin and soft tissue infections within 90 days in patients with beta-lactam allergy labels treated with either cefazolin or second line agents.7
This was a single center retrospective chart review of beta-lactam allergic adult patients who underwent total knee arthroplasties (TKA) or total hip arthroplasties (THA).7 Beta-lactam allergy histories were categorized into immediate, delayed, or undetermined based on documented symptoms. Immediate reactions included anaphylaxis and hives. Delayed reactions included pruritus and blood cell dysfunction such as neutropenias.7
The primary outcome was SSI, defined by the CDC and NHSN. The SSI was reviewed and confirmed by an orthopedic surgeon. Secondary outcomes included interoperative hypersensitivity reactions (HSRs), which are defined as hemodynamic instability (systolic blood pressure [SBP] < 80 mm Hg or > 40% SBP reduction), interoperative receipt of epinephrine and/or diphenhydramine, or a new documented allergy in the chart after receipt of a perioperative antibiotic.7
The study included 2 study arms based on perioperative antibiotics received comparing cefazolin vs clindamycin and/or vancomycin. A total of 1100 total hip or knee arthroplasties were required to meet power. There were 809 patients who had received cefazolin and 319 patients who had received clindamycin and/or vancomycin (alternative antibiotics).7
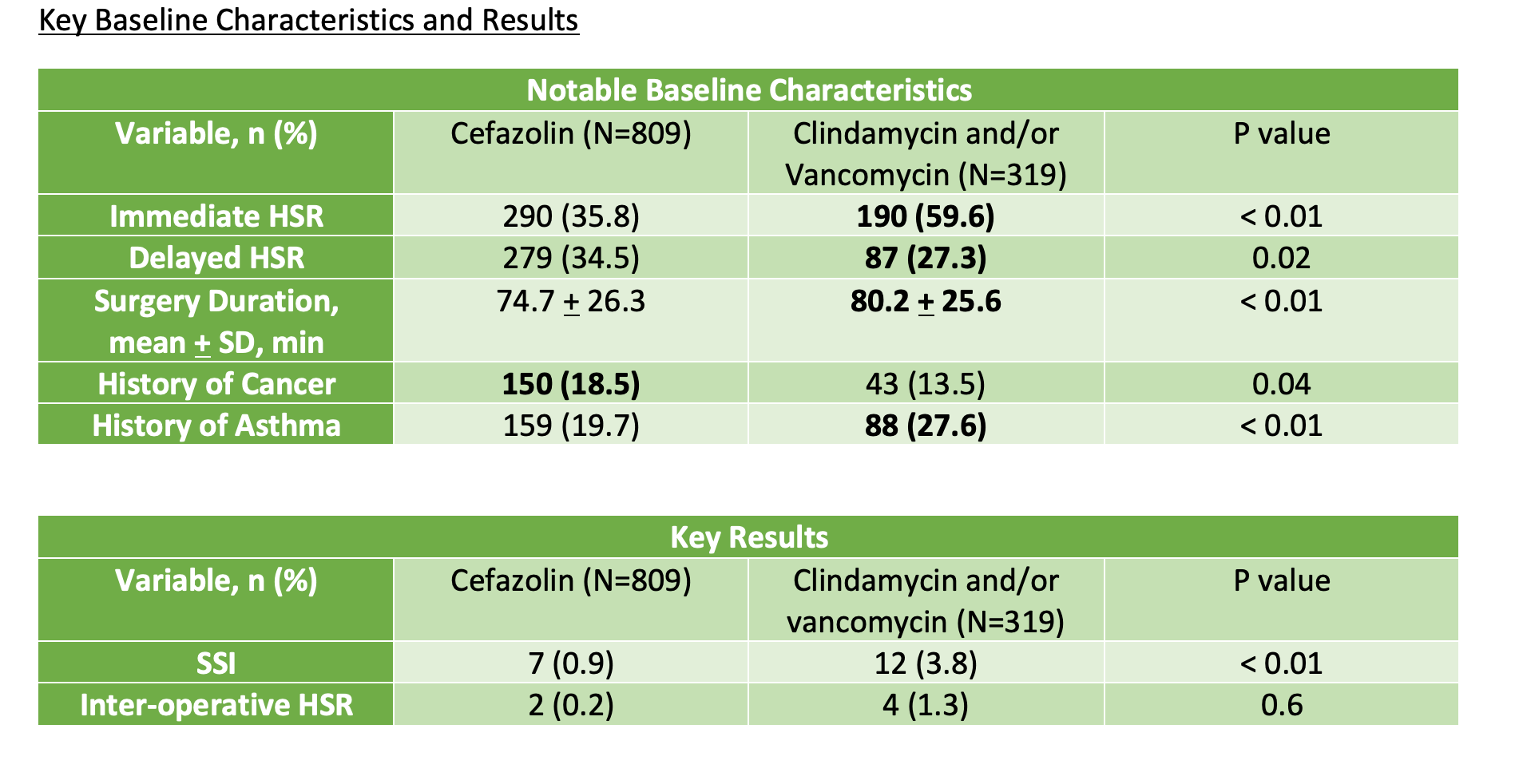
In patients receiving cefazolin, there were significantly fewer incidences of SSI when compared with patients receiving alternative antibiotics (7 [0.9%] v 12 [3.8%]; P<0.01). The lower SSI rates seen in the cefazolin group were not associated with increased inter-operative HSR (2 [0.2%] v 4 [1.3%]; P=0.6).7 However, in patients who had received alternative antibiotics, more patients had a history of immediate HSR to beta-lactam antibiotics (cefazolin: 290 [35.8%] vs alternative: 190 [59.6%]; P<0.01) and a history of asthma (cefazolin: 159 [19.7%] vs alternative: 88 [27.6%]; P<0.01). The imbalance in baseline characteristics for immediate HSR history and asthma history would put patients at increased risk of having an HSR.7 Nevertheless, the results are supported by a 2019 study investigating prosthetic joint infections comparing cefazolin with second line antibiotics in patients undergoing TKA or THAs. Investigators found significantly more infection free patients receiving cefazolin vs patients receiving alternative antibiotics (P < 0.001).6
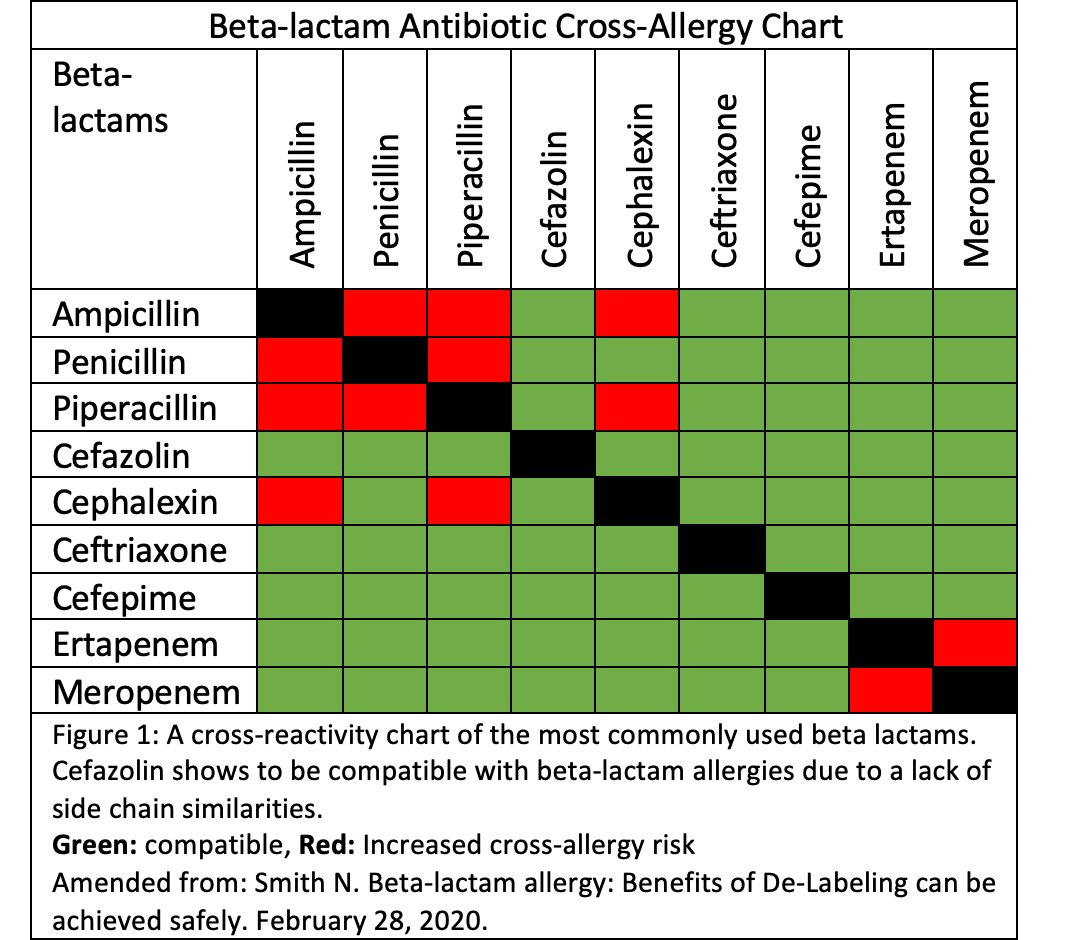
Beta-lactam side chains are the culprit for cross-reactivity across the beta-lactam family. Because cefazolin does not share similar chains with penicillin type antibiotics or other cephalosporins, cefazolin can be considered as a viable agent for surgical prophylaxis (Figure 1). Patients receiving cefazolin demonstrated similar rates of HSR compared with clindamycin and/or vancomycin. The low HSR rates in this study may be due to lack of similar side chains to other beta-lactams and the loss of beta-lactam hypersensitivity over time.5,8 As of July 2023, there is a national shortage of intravenous clindamycin, which will raise questions for alternatives for surgical prophylaxis in beta-lactam allergic patients. Results from this study as well as others support the use of cefazolin in beta-lactam allergic patients.
References
1. Bratzler DW, Dellinger EP, Olsen KM, et al. Clinical practice guidelines for antimicrobial prophylaxis in surgery. Surg Infect (Larchmt). 2013;14(1):73-156. doi:10.1089/sur.2013.9999
2.Surgical site infection - centers for disease control and prevention. Accessed July 23, 2023.
3. Norvell MR, Porter M, Ricco MH, et al. Cefazolin vs Second-line Antibiotics for Surgical Site Infection Prevention After Total Joint Arthroplasty Among Patients With a Beta-lactam Allergy. Open Forum Infect Dis. 2023;10(6):ofad224. Published 2023 Apr 24. doi:10.1093/ofid/ofad224
4. Stone CA Jr, Trubiano J, Coleman DT, Rukasin CRF, Phillips EJ. The challenge of de-labeling penicillin allergy. Allergy. 2020;75(2):273-288. doi:10.1111/all.13848
5. Romano A, Gaeta F, Valluzzi RL, Zaffiro A, Caruso C, Quaratino D. Natural evolution of skin-test sensitivity in patients with IgE-mediated hypersensitivity to cephalosporins. Allergy. 2014;69(6):806-809. doi:10.1111/all.12390
6. Wyles CC, Hevesi M, Osmon DR, et al. 2019 John Charnley Award: Increased risk of prosthetic joint infection following primary total knee and hip arthroplasty with the use of alternative antibiotics to cefazolin: the value of allergy testing for antibiotic prophylaxis. Bone Joint J. 2019;101-B(6_Supple_B):9-15. doi:10.1302/0301-620X.101B6.BJJ-2018-1407.R1
7. Miranda R Norvell and others, Cefazolin vs Second-line Antibiotics for Surgical Site Infection Prevention After Total Joint Arthroplasty Among Patients With a Beta-lactam Allergy, Open Forum Infectious Diseases, Volume 10, Issue 6, June 2023, ofad224, https://doi.org/10.1093/ofid/ofad224
8. Smith N. Beta-lactam allergy: Benefits of De-Labeling can be achieved safely. February 28, 2020. Accessed July 11, 2023.
Newsletter
Stay ahead of emerging infectious disease threats with expert insights and breaking research. Subscribe now to get updates delivered straight to your inbox.
